 In comparison, the rate in sinus tachycardia normally fluctuates somewhat from beat to beat, but the rate in AVNRT/AVRT is frequently quicker (170-250 bpm).Suspect atrial flutter with 2:1 block anytime a regular narrow-complex tachycardia at 150 bpm occurs - especially when the rate is exceedingly constant.By contrast, atrial fibrillation is characterised by total irregularity, with no discernible patterns within the R-R intervals.Look for similar R-R intervals that occur intermittently throughout the rhythm strip then, determine if the various R-R intervals on the ECG have a mathematical connection.R-R intervals in an atrial flutter with variable block will be multiples of the P-P interval - for example, given an atrial rate of 300 bpm (P-P interval of 200 ms), the R-R interval would be 400 ms with 2:1 block, 600 ms with 3:1 block, and 800 ms with 4:1 block.Unlike AVNRT, these procedures do not often cardiovert atrial flutter, but a transitory period of enhanced AV block may reveal flutter waves. Invert the ECG and carefully inspect the inferior leads (II, III + aVF) for flutter waves.Is there a narrow complex tachycardia at 150 beats per minute (range 130-170)? If yes-> Flutter is a possibility.Is often linked with increased atrial rates and rhythm instability.Does not meet the criteria for typical atrial flutter.Atypical atrial flutter (uncommon, or type II atrial flutter) Flutter waves that are positive in leads II, III, and aVFĢ.This unusual variation results in the inverse pattern : In V1, positive flutter waves resemble upright P waves.Flutter waves inverted in leads II, III, and aVF.This atrial flutter is the most common kind (90 per cent of cases). It can be categorised further on the direction of the reentry circuit (anticlockwise or clockwise). The reentry circuit is comprised of the IVC and tricuspid isthmus. Typical atrial flutter (common, or type I atrial flutter) This is based on the anatomical position and direction of the re-entry circuit. AV block is a physiological reaction to rapidly increasing atrial rates and indicates that the AV node is working correctly. The phrase "AV block" is a misnomer when used to atrial flutter. Atrial flutter with 1:1 conduction is linked with significant hemodynamic instability and ventricular fibrillation development.Treatment with AV-nodal blocking medications in a patient with WPW may trigger this. Atrial flutter with 1:1 conduction may develop as a result of sympathetic stimulation or when an auxiliary route is present.Higher-degree blocks, often caused by drugs or underlying cardiac disease, may develop, resulting in decreased ventricular conduction rates, e.g.The most often used AV ratio is 2:1, which results in a ventricular pace of 150 beats per minute. The AV conduction ratio ("degree of AV block") is used to calculate the ventricular rate. 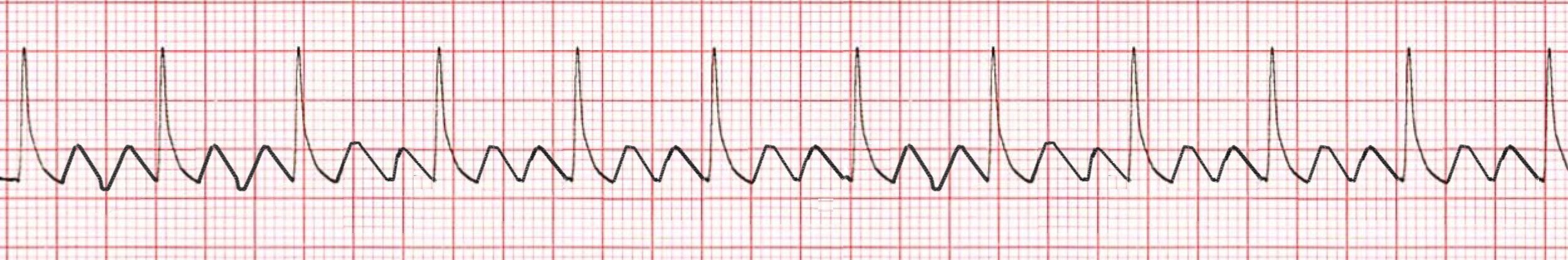
The length of the re-entry circuit is proportional to the size of the right atrium, resulting in a rather predictable atrial rhythm of around 300 beats per minute (range 200-400). Atrial flutter is a kind of supraventricular tachycardia generated by a right atrial re-entry circuit.Upon closer examination, a pattern of alternating 2:1, 3:1, and 4:1 conductor ratios may be seen.Ītrial flutter pathophysiologic mechanisms.The ventricular response is erratic, resembling AF.In comparison to the heart's atrial pace, the ventricular rate is just a small portion like: It is important to note that the aforementioned pattern of inverted flutter waves in inferior leads and upright flutter waves in V1 occurs in 90% of instances of atrial flutter caused by anticlockwise re-entry. The ventricular rate is influenced by the AV conduction ratio (refer to the image below).Upright flutter waves in V1 that may mimic P waves."Saw-tooth" pattern of inverted flutter waves in leads II, III, and aVF.Regular atrial activity at 300 beats per minute.AF may result in potentially fatal complications such as stroke and heart failure. The worry is a lack of documentation or identification of AF and its accompanying symptoms. AF is difficult to detect since it is often asymptomatic and requires a battery of tests to establish the diagnosis. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
